Obesity in Dogs: Signs, Causes, and Treatment
Just like people, dogs can struggle with weight gain—and it can be hard to notice when those extra pounds start adding up.
Obesity in dogs is more than just a cosmetic issue; it can lead to serious health problems and shorten your dog’s lifespan.
Understanding the risks, causes, and ways to manage obesity can help you keep your dog healthy for years to come.
Key Takeaways
- ~65% of dogs are considered overweight or obese in the U.S.
- Obesity in dogs can lead to serious health issues like arthritis, kidney disease, and respiratory problems, all which can shorten a dog’s lifespan.
- Overfeeding, lack of exercise, and certain medical conditions such as hypothyroidism and Cushing’s disease are common causes of obesity.
- Managing obesity involves a combination of dietary changes, increased physical activity, and regular veterinary monitoring to ensure weight loss is done safely.
What is Obesity in Dogs?
Obesity can be defined as an excess accumulation of body fat that contributes to disease.
Dogs that weigh at least 10% above their ideal body weight are considered overweight, while dogs weighing 20% more than ideal are considered obese.
Excess body weight can be a contributing factor in many diseases.
Risks Associated With Obesity in Dogs
Up to 65% of dogs in the U.S. are considered overweight or obese. Obesity can contribute to many health issues in dogs, including:
-
Respiratory compromise
-
Decreased exercise and heat tolerance
-
Increased risk of cardiovascular disease
-
Abnormal response to insulin
-
Increased anesthetic risk
-
Decreased quality of life
Showing love by showering your dog with treats may result in a shortened lifespan and decreased quality of life if the excess calories result in obesity.
Symptoms of Obesity in Dogs
Signs of an overweight dog may include:
-
Weight gain
-
Less energy than usual
-
Decreased exercise tolerance
-
A collar or harness that seems tighter than it used to be
-
Being unable to feel the ribs, or seeing a “waistline” (a small tuck in the belly right in front of the hind legs)
Health Tools
Get quick answers with our vet-created Symptom Checker
Causes of Obesity in Dogs
The most obvious cause of obesity in dogs is overfeeding, which can include the dog’s regular wet or dry food, treats designed for dogs, and table scraps or human foods.
Inadequate exercise can also lead to your dog becoming overweight. Additionally, there are some medical conditions that cause obesity, including hypothyroidism and Cushing’s disease.
Certain dog breeds can also be predisposed to obesity, including:
Is My Dog Overweight?
If you suspect your dog may be overweight, schedule a weight check and examination with your veterinarian.
If there seems to be excess padding over your dog’s ribs or you are unable to see a slight tuck-up just in front of the hind legs, chances are high that your dog is carrying excess weight.
How Veterinarians Diagnose Obesity in Dogs
Your veterinarian can obtain your dog’s weight and look for trends over time indicating weight gain or loss. A measurement called body condition scoring is typically done at this time.
The two most commonly used body condition scores are a five-point scale (where three is considered ideal) and a nine-point scale (where four to five is considered ideal). Your dog should have an hourglass shape when viewed from above if they are at their ideal body weight, which can be determined through their body condition score.
Body Condition Score Based on Dog Size
Small Dog
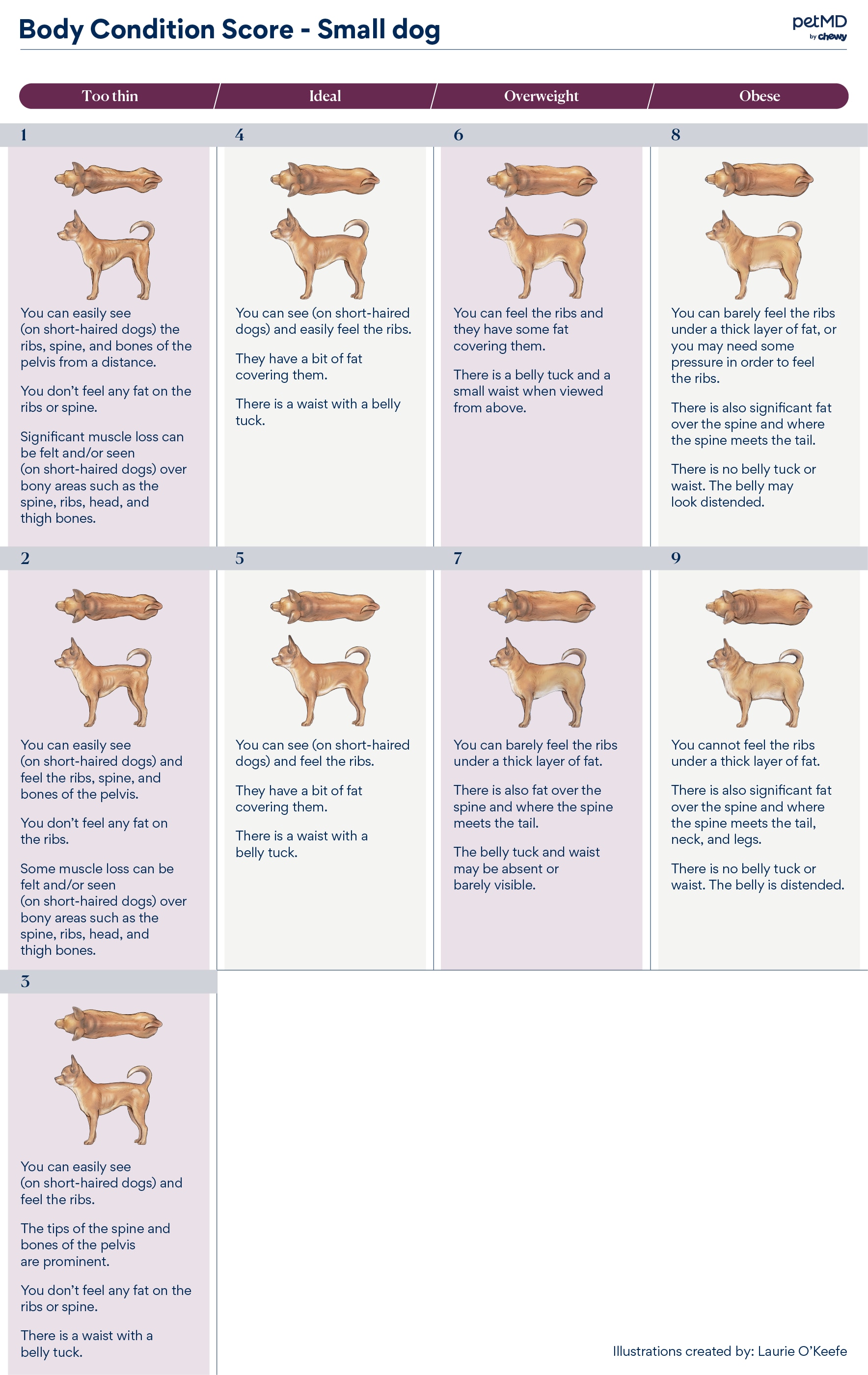
Click here to download this medical illustration.
Medium-Sized Dog
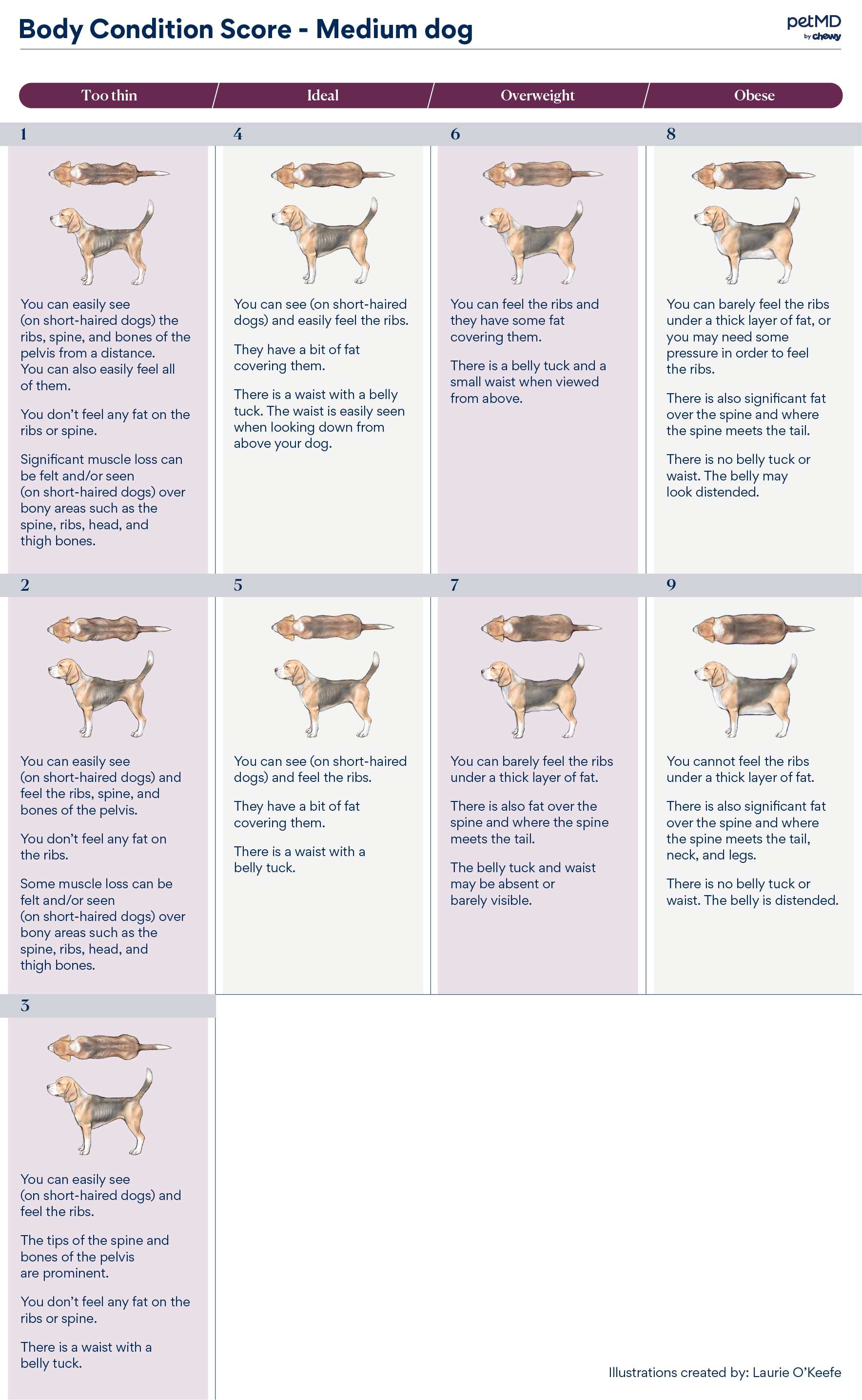
Click here to download this medical illustration.
Large Dog

Click here to download this medical illustration.
Extra-Large Dog

Click here to download this medical illustration.
Your veterinarian may also run some blood work to check for any underlying conditions that may be contributing to weight gain, such as hypothyroidism or Cushing’s disease.
If the weight gain has been very sudden, your veterinarian may also recommend X-rays to check for fluid or masses in the abdomen.
Treatment of Obesity in Dogs
The basic components for treating obesity are exercise and dietary changes.
Exercise
Depending on the severity of obesity and current fitness level, increasing the amount of your dog’s daily exercise may need to be done gradually.
In general, most dogs can safely exercise for 15–30 minutes per day to start. The duration and intensity can be slowly increased as your dog loses weight and becomes more fit.
A simple walk is feasible for most families, but exercise can also include playing fetch indoors or outdoors, swimming, and running.
If your dog is older, you’ll need to follow a senior-specific exercise plan depending on their health.
Diet
Dietary changes should be made with the guidance of your dog’s veterinary team. The reduction or elimination of extras like treats and table scraps will be helpful, and a change in type and/or amount of food is often needed.
There are many weight loss diets available. Some options, like Blue Buffalo True Solutions Natural Weight Control Dry Dog Food and Blue Buffalo True Solutions Natural Weight Control Wet Dog Food, are available over the counter.
Other weight loss diets can only be purchased with authorization from your veterinarian.
Since dogs who are overweight and obese are at a higher risk of other comorbidities, some veterinary weight loss diets target multiple issues at once, like Blue Buffalo Natural Veterinary Diet Weight Management + Mobility Support and Blue Buffalo Natural Veterinary Diet Weight Management + Urinary Care.
Other commonly recommended weight loss foods for dogs include:
A good goal is weight loss of 1–2% of body weight per week, ideally reducing body fat stores while maintaining lean body tissue.
Feeding Recommendations
While most dog foods give feeding amount recommendations, these are only guidelines, and individual dogs may need more or less than recommended to maintain ideal body condition.
Meal feeding (instead of just leaving a full bowl without measuring) is often helpful in controlling caloric intake. It is also important to use a measuring dog food scoop to ensure consistent feeding of the appropriate amount of food. Splitting your dog’s daily calories into two meals a day is generally recommended for most dogs.
Instead of eliminating treats completely, you may opt to switch to baby carrots, frozen green beans, pumpkin, or lower-calorie dog treats like Hill’s Prescription Diet Metabolic Crunchy Dog Treats, if your veterinarian agrees that these are good options for your dog.
Medications are not typically needed to treat obesity unless your dog has Cushing’s disease or hypothyroidism, in which case regular exams and lab tests will help determine the appropriate type and dose of medication.
Recovery and Management of Obesity in Dogs
Once your dog has reached their ideal weight, your veterinarian may recommend transitioning to a maintenance diet.
A maintenance diet is one that allows a dog to maintain their new weight without packing on the pounds like a regular dog food would cause after being on a weight loss diet.
It is important to continue regular exercise and limit extra treats and snacks.
Prevention of Obesity in Dogs
Of course, preventing obesity in your dog before it even happens is ideal. This can be achieved by offering two meals per day instead of always having food available, avoiding excessive treats, and ensuring that your dog gets regular exercise.
In some cases, your vet may recommend feeding your dog three times a day especially in cases related to extra small breeds, certain senior dogs, or puppies.
Exercise is not just good for your dog—it’s good for humans too— and offers physical and emotional benefits for all involved.
While it takes effort to prevent or correct obesity, the benefits of a longer and healthier life are well worth it for you and your dog
Obesity in Dogs FAQs
What are the symptoms of obesity in dogs?
The signs of obesity in dogs include weight gain, extra fat coverage over the ribs, and lack of a natural waist at the end of the ribs. Some obese dogs have more of a round belly, and extra rolls by their tail and neck. Other symptoms of obesity in dogs include lethargy, exercise intolerance, high blood pressure, excessive panting, and mobility changes.
How do you manage obesity in dogs?
Obesity in dogs is managed with dietary changes and increased exercise. Weight loss diets for dogs can be obtained over the counter or through a prescription from your vet. Weight loss diets for dogs are available in both wet and dry formulas. Increased exercise can mean longer or more rigorous walks, extra playtime in the yard, or even a doggy treadmill.
What is the quickest way for a dog to lose weight?
The quickest way for a dog to lose weight is by a strict diet low in calories while still providing adequate nutrients and a full belly. Adding extra walks and more exercise also helps a dog lose weight. Always work with your vet when helping your dog to lose weight so that it is done safely.
What dog breed is most prone to obesity?
Dog breeds that are prone to obesity include Labrador retrievers, Golden retrievers, Cocker spaniels, Dachshund, Beagle, Boxer, and Pugs.
