Bobcat Fever in Cats: Symptoms, Treatment, and Prevention
Berk Ucak/iStock/Getty Images Plus via Getty Images
What Is Bobcat Fever in Cats?
Bobcat fever is a deadly tick-borne disease. Also known as cytauxzoonosis, bobcat fever is caused by a protozoa parasite called Cytauxzoon felis. While the parasite is harmless in bobcats, it’s extremely dangerous to cats.
Affected felines will become lethargic, get anemia, and spike a fever, often dying within a couple weeks of their tick bite.
Bobcat fever is always considered a medical emergency. It’s important to act quickly to save a cat infected by cytauxzoonosis.
Key Takeaways
- Bobcat fever (cytauxzoonosis) is a life-threatening tick-borne disease in cats, caused by Cytauxzoon felis.
- Symptoms like lethargy, poor appetite, and high fever progress rapidly and can be fatal within days.
- Fast veterinary treatment improves survival, but year-round tick prevention and keeping cats indoors offer the best protection.
Causes of Bobcat Fever in Cats
Bobcat fever in cats is caused by a protozoa parasite, C. felis. The protozoa are carried by many bobcats, with up to 80% of bobcats being carriers in some regions. Bobcats that are infected with the parasite have no symptoms of disease.
After ticks feed off bobcat carriers, they spread the disease when they attach themselves to cats.
The disease is usually spread by the Lone Star tick but can be spread by the American dog tick as well.
Cats who have been bitten by a tick will not show signs of disease for 10–14 days. After the incubation period, they will act lethargic and not eat well. The disease moves rapidly from there to a fever, with many cats dying two to three days after they get the fever.
Outdoor cats who live near wooded areas or other bobcat habitats are at the highest risk of getting bobcat fever. Indoor-only cats who live with other pets who go outdoors and can carry ticks inside are also at risk of getting cytauxzoonosis.
Bobcats are more common in the Southeast, South Central, and Midwest parts of the United States. The Lone Star tick is also prevalent in these areas, making outdoor/indoor cats who live in these locations at the highest risk of getting bobcat fever.
How Veterinarians Diagnose Bobcat Fever in Cats
Veterinarians use the following techniques to diagnose bobcat fever in cats:
-
Physical exam. Your vet will take your cat’s temperature to look for a fever and check how hydrated they are. They will also look for things like pale gums, increased respiratory (breathing) rate or heart rate, and enlarged lymph nodes. They will feel your cat’s belly for any organ enlargement or signs of pain.
-
Blood work. Labs will be pulled to look for changes in the red blood cells, white blood cells, platelets, and organs that would point toward a tick-borne illness.
-
Blood smear. A small amount of blood can be smeared on a slide for a pathologist to look for evidence of these tiny parasites in your cat’s blood.
-
PCR testing. Blood can be sent to a lab to look for genetic material of C. felis.
-
Imaging. Your vet may recommend imaging (like X-rays or an ultrasound) to rule out other causes of disease that can look similar.
Treatment of Bobcat Fever in Cats
Bobcat fever in cats is curable, but because it worsens quickly, it only carries a 60% survival rate.
If your cat is diagnosed with bobcat fever, they will be treated aggressively with a combination of two medications, atovaquone (a drug used to treat malaria and a serious form of pneumonia) and azithromycin (an antibiotic).
In addition to these two medications, your cat will need supportive care while their body is trying to fight the infection. Many cats are hospitalized for a week or more. While in the hospital, they may be on IV fluids and have a feeding tube placed.
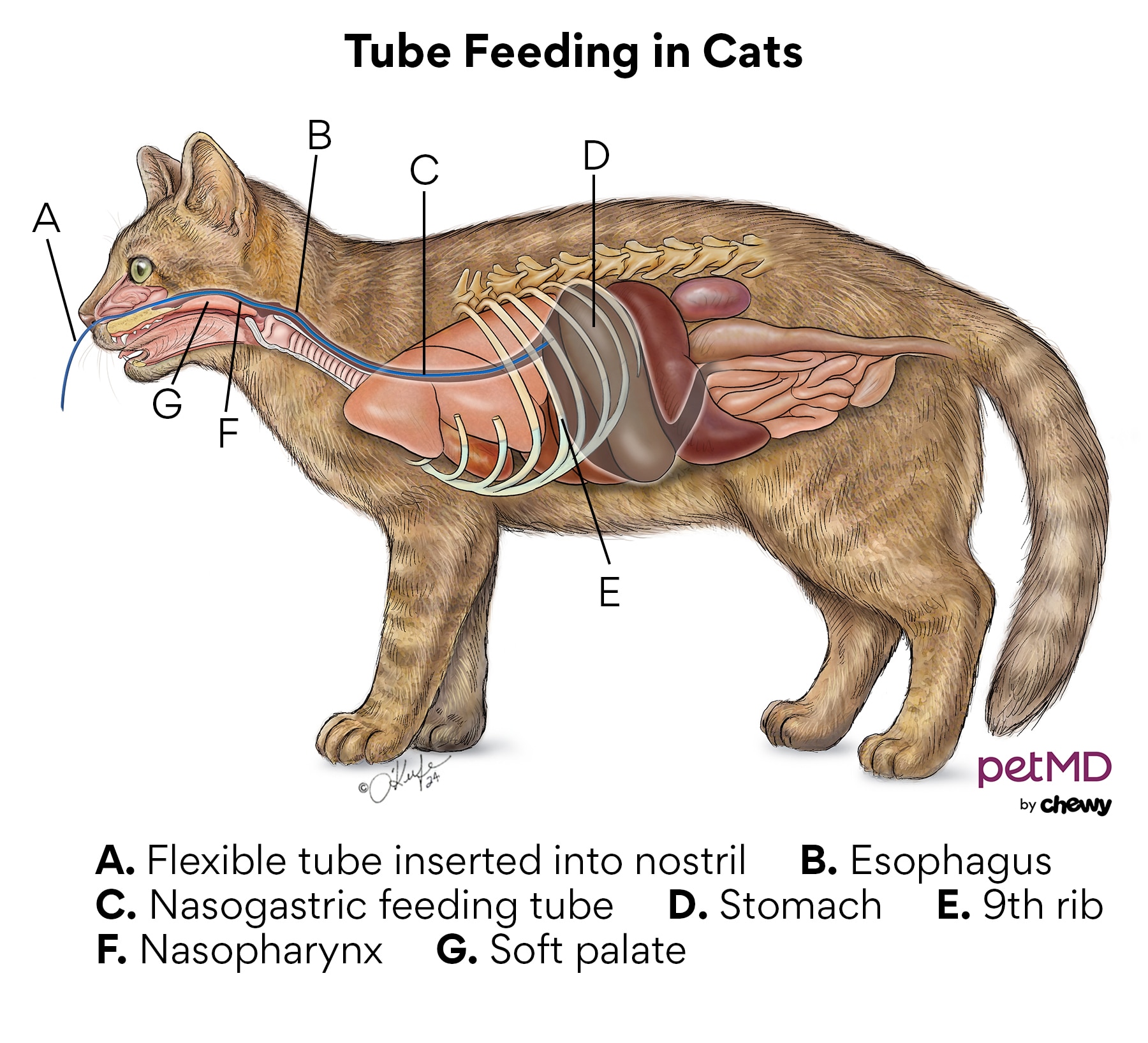
Click here to download this medical illustration.
Some cats have such severe anemia that they need to be in an oxygen cage and may need blood transfusions.
Recovery and Management of Bobcat Fever in Cats
When bobcat fever is caught quickly and treated aggressively, affected cats can recover. Recovery usually takes one to two weeks.
Your cat may come home with a feeding tube if nutritional support is needed. Diets that are nutrient-dense and readily slurried, like Hill’s a/d Urgent Care or Royal Canin Recovery, make good options for these pets.
After being on strong antibiotics and anti-malarial medication, your cat may have some stomach upset. Probiotics like Purina FortiFlora and Cerenia can help them get their digestive system back on track.
Injectable B12 can help anemic cats make more red blood cells.
Pet parents who feel comfortable giving injections under the skin can talk to their vets about starting weekly injections.
Recovered cats are considered carriers for life and shouldn’t be allowed outdoors.
While the infection can’t spread from cat to cat, it’s spread by ticks feeding off a carrier before biting another cat.
Not giving ticks access to the carrier cat helps to stop further spread.
Prevention of Bobcat Fever in Cats
The surest way to prevent bobcat fever in cats is to keep them indoors and not exposed to any ticks.
A high-quality flea/tick prevention product, like NexGard Combo or Bravecto Plus, can help protect cats from getting ticks.
Tick prevention is very important in cats who go outdoors and is helpful even for cats who are indoors but are near dogs who go outdoors.
Be sure to thoroughly check your cat over daily for ticks, especially during the peak months of March through September.
Bobcat Fever in Cats FAQs
What are the symptoms of bobcat fever in cats?
The most common symptoms are lethargy and decreased appetite, followed by a fever.
How long do cats live with bobcat fever?
Without veterinary treatment, once cats get symptoms they will live only for a few days.
Is bobcat fever contagious to humans?
No, bobcat fever is not contagious to humans.
How do cats catch bobcat fever?
Cats catch bobcat fever from being bitten by a tick that fed first from an infected bobcat.
