Insulin For Dogs and Cats: What Is It and How to Give Your Pet a Shot
SPONSORED BY
Chalabala/iStock via Getty Images
This article is sponsored by UltiCare® VetRX. It is provided for educational purposes only and is not intended to be a substitute for professional and/or medical advice. For specific guidance on how to give an injection to your pet, talk to your veterinarian.
If your dog or cat has diabetes, you may have been told they need to take insulin. Insulin for dogs and cats helps regulate blood sugar levels and is typically administered via injection.
The thought of giving your dog or cat an insulin shot may seem a little intimidating at first, and that’s perfectly normal. Using the proper tools, like UltiCare® VetRX’s insulin syringes, and educating yourself on how to give a dog or cat an insulin shot can help give you the confidence to successfully manage your pet’s condition.
But first, let’s walk through what insulin is and how it helps diabetic pets.
What Is Insulin?
Insulin is a hormone made naturally by the pancreas. It helps the body turn sugar from food into energy. Lack of insulin leads to high blood sugar levels and eventually diabetes.
Signs of diabetes in dogs and cats:
-
Increased thirst
-
Increased urination
-
Increased appetite
-
Weight loss
-
Lethargy or weakness
Insulin administered to diabetic pets is an injectable version of the hormone normally produced by your pet's pancreas. Insulin is generally synthesized using recombinant DNA or purified from animal sources, like pigs and cows.
How Does Insulin for Dogs and Cats Work?
Insulin helps move sugar molecules, aka glucose, from the bloodstream and into the cells where it can be used to make energy.
Glucose comes from the food our pets eat. When they eat, their digestive system breaks the food down into simpler sugars which are then absorbed into the bloodstream.
Insulin helps shift the sugar from the blood into the cells where it can be used to create energy, thereby lowering the level of glucose in the bloodstream.
Understanding Your Dog or Cat’s Insulin Prescription
There are many kinds of insulin on the market. When treating an uncomplicated diabetic pet, your veterinarian typically selects an insulin based on efficacy in the species, duration of action, and concentration. They’ll also prescribe a specific dosage for your pet.
Concentration
The most important distinction is that insulin comes in two different concentrations: 40 units of insulin per milliliter (40 U/mL) or 100 units of insulin per milliliter (100 U/mL). The concentration is specific to the specific insulin.
For example, ProZinc is a U-40 insulin, meaning the concentration is 40 units of insulin per 1 mL, whereas glargine is a U-100 insulin, meaning the concentration is 100 units of insulin per 1 mL.
Syringes come in two sizes that match the insulin concentrations U-40 and U-100. The syringes will be labeled U-40 or U-100.
It is critical that your insulin syringes match the concentration of the insulin that you have for your pet. Utilizing the incorrect syringe type will cause your pet not to receive the proper dose of insulin.
For example, UltiCare VetRX’s U-40 insulin syringes should only be used with U-40 (40 units per mL) insulin in pets with diabetes. And UltiCare VetRX’s U-100 insulin syringes should only be used with U-100 (100 units per mL) insulin in pets with diabetes.
Insulin Source
As noted above, insulin for pets comes from the pancreas of pigs or cows.
Porcine (pig) based insulin: Since dog and pork insulin are essentially the same molecule, porcine based insulins like Vetsulin® or VetPen® are typically recommended for use in diabetic dogs. Other options like NPH (Humulin® or Novolin®) insulin are also commonly used in dogs.
Bovine (cow) based insulin: Cat insulin molecule more closely resembles bovine (cow) insulin. Since protamine zinc insulin (ProZinc®) and glargine insulin (Lantus®) are made from bovine insulin, either of these is often recommended in diabetic cats to control their blood sugar levels and achieve diabetic remission.
Other common insulin medications prescribed for dogs and cats include Levemir®, NovoLog®, and Humalog®.
While only Vetsulin®, and ProZinc®, are FDA-approved, the others are readily utilized in the veterinary field, and veterinarians can legally prescribe certain human drugs in animals in certain circumstances. This is called extra-label or off-label use because this use isn’t described on the drug label.
Duration
If insulin will be given at home, most pets are prescribed intermediate or long-lasting insulin. Typically, these insulins last 12–24 hours depending on the specific insulin. Your vet will provide specific administration recommendations for your pet, but often insulin in pets is given twice per day with meals.
Regular or short-acting insulin are mostly used only in a hospital. This is because these insulins need to be administered as frequently as every two hours or even on an intravenous (IV) drip.
Dosage
If your pet is a newly diagnosed diabetic, your veterinarian will likely start them on insulin at a dosage determined by their weight.
The specific protocols can vary, but frequent recheck visits will be needed for newly diagnosed diabetic pets as your vet works to dial in the best dosage of insulin to control your specific pet’s blood sugar.
Often this involves a test called a glucose curve in which your veterinarian measures your pet’s blood sugar every two to four hours over an eight- to 12-hour period to determine the effect the insulin is having on your pet’s blood sugar throughout the day.
Based on this curve, the veterinarian will likely adjust the insulin dosage until they find the best dosage for your pet.
Typically, once a newly diagnosed diabetic is stabilized and on the best dosage of insulin, they will remain on that dosage with periodic monitoring.
The dosage of insulin will be given in units that will match the syringe. For example, if the dosage is 5 units, you will draw the syringe back to the 5-unit mark on the syringe.
Remember, it is very important to make sure the concentration of the insulin (U-40 or U-100) matches the syringe (U-40 or U-100).
Let's look at a 1 mL U-40 syringe and a 1 mL U-100 syringe. Even though they are both the same size syringe, there would be less marks on the U-40 syringe (only 40) and more marks (100 of them) on the U-100. That means the U-40 markings would be more spread out and the U-100 marks would be closer together.
Giving a dosage of 5 units would look very different in each syringe; 5 units on a U-40 syringe would be a larger volume of insulin vs 5 units on a U-100 syringe.
To help differentiate U-40 syringes typically have a red cap:
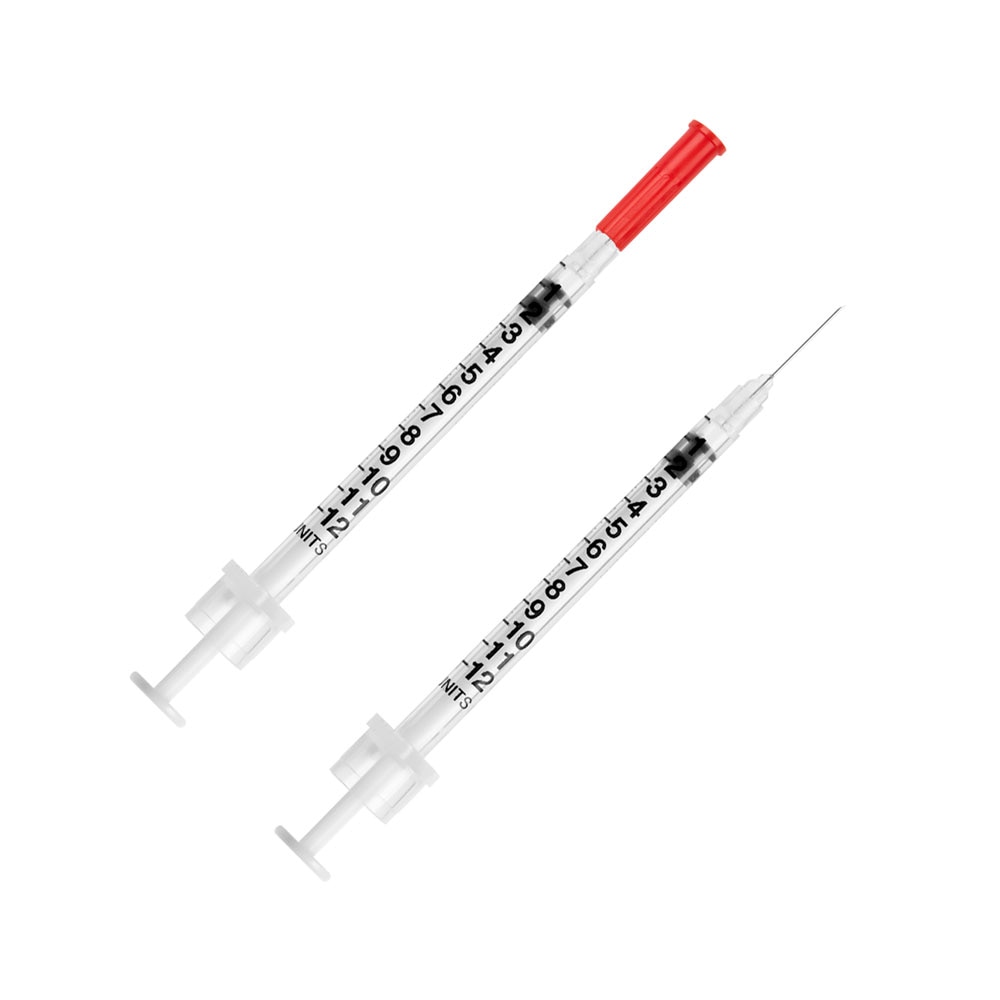
U-100 syringes typically have an orange cap:
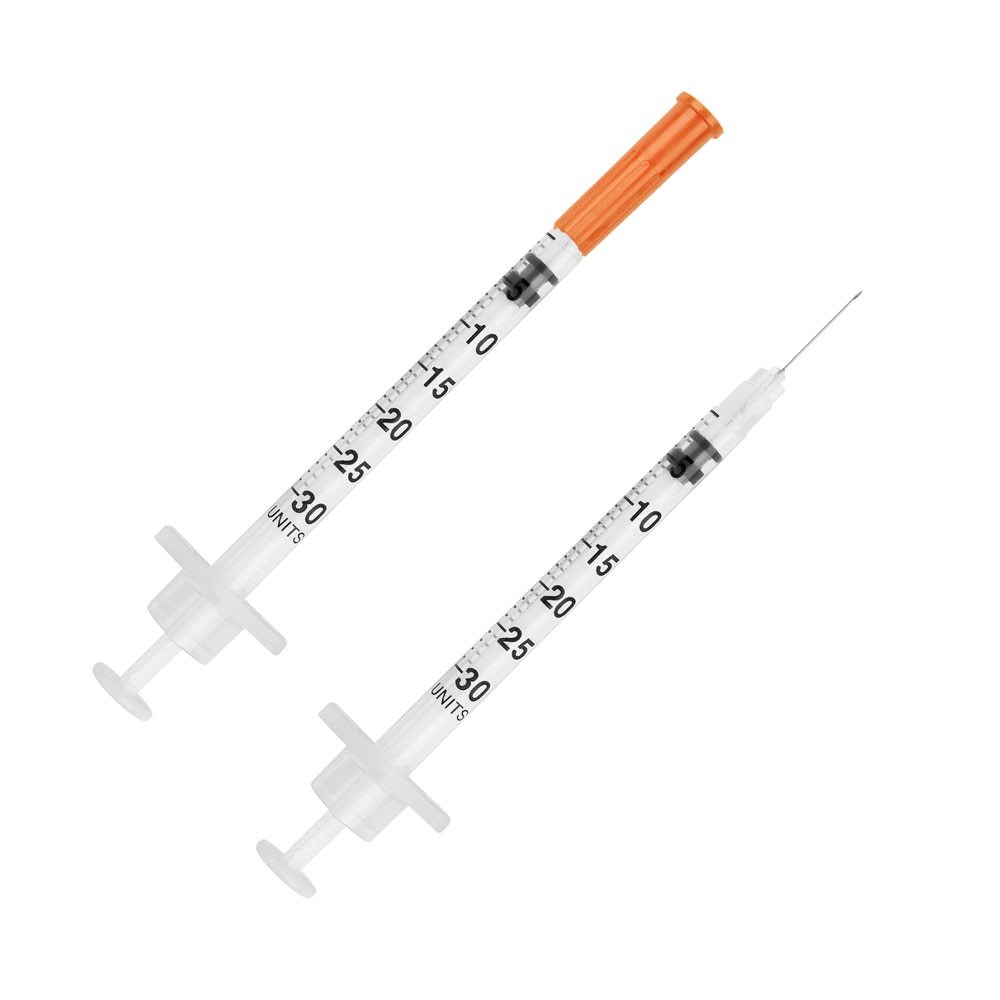
How to Give a Dog or Cat an Insulin Shot
It is very important that you follow the directions provided by your veterinarian. Most pets will need to be given insulin injections twice a day and will be started at a dose based on your pets' weight.
Consistent timing, feeding, and treatment are essential for the management of diabetes in dogs and cats.
General recommendations for how to give a dog or cat insulin via vial include:
- Ensure that your pet has eaten sufficiently before administering insulin. (If your pet does not eat a full meal or does not eat at all, please contact your vet for instructions.)
- Clean the top of the insulin vial with an alcohol wipe. Roll the vial in between your hands to mix until the insulin appears uniform in color/consistency. Do not shake the vial.
- Draw up the prescribed amount of insulin in a new syringe. Do not touch the needle. Ensure that your insulin syringe matches your pet’s type of insulin. Accurate measuring of insulin is key.
- Cat and dog insulin injections are given just under the skin. Alternating injection locations helps to avoid soreness at the injection site.
- Have someone help you hold your pet or distract them with a low carb treat. (Opt for a low-carb treat, because carbohydrates are easily broken down into glucose, or sugar, and then quickly absorbed, which can cause blood sugar spikes.)
- Hold the pet syringe in one hand and with the other pinch a section of skin into a tent type shape. Insert the needle confidently into the center of the tent.
- Once the needle is under the skin, gently push the syringe plunger all the way down to dispense all the insulin.
- Carefully withdraw the needle from the skin and dispose of the pet syringe and needle into an appropriate sharps container (see more on that below).
Download this step-by-step guide for giving your pet an insulin injection.
For general recommendations for administration of insulin via insulin pen, you should follow the manufacturer’s instructions and ask your vet.
Proper Disposal of Dog and Cat Insulin Needles
Place all needles in a sharps disposal container immediately after they have been used.
UltiCare VetRX’s UltiGuard SafePacks pull double duty by housing syringes to be used in one compartment and providing a storage container for the syringes after they are used.
Keep the container out of reach of children and pets.
Once full, dispose of the used needles and syringes in accordance with all federal, state and local environmental laws.
Possible Side Effects of Insulin for Dogs and Cats
The most common side effect of dog and cat insulin is low blood sugar (hypoglycemia).
If a pet’s blood sugar levels drop too low, it can be a life-threatening emergency.
If you see any of the following symptoms, please contact your veterinarian immediately:
- Weakness/disorientation/stumbling
- Lack of energy/lethargy
- Lack of appetite
- Vomiting
- Shaking, tremors, or muscle twitching
- Collapse
- Seizure
- Coma
Additional symptoms related to general symptoms of diabetes in dogs and diabetes in cats are also possible.
Insulin Side Effects in Humans
If you accidentally inject yourself with this medication, call your physician or the national Poison Control Center hotline at 800-222-1222.
Cat or Dog Insulin Overdose
Signs of an overdose of insulin are generally a result of hypoglycemia, or a blood sugar level that has fallen too low. If you notice any of the symptoms of hypoglycemia listed above, please contact your veterinarian or local emergency clinic immediately.
Mild hypoglycemia may be treated by having your pet eat an additional meal. However, more serious symptoms should be treated in a hospital by a veterinarian.
If you suspect an overdose, or you accidentally gave your pet insulin an extra dose, please immediately contact your veterinarian or an animal poison control center. Consultation fees often apply.
- Pet Poison Helpline®: 855-764-7661
- ASPCA Animal Poison Control®: 888-426-4435
Missed a Dose?
A missed dose (or an inadequate dose) may cause temporary recurrence of signs of diabetes (like increased drinking and urination), but it is not life-threatening.
Contact your vet as soon as possible for advice on your dog or cat’s next dose. If you can’t get in touch with your vet and your pet is eating and acting normal, give your pet the usual dose at the next regularly scheduled injection time.
Do not give extra or double doses—this can cause life-threatening side effects.
If you think you did not inject all of the insulin dose into the subcutaneous space under the skin or it seems that some of the insulin came back out, the safest option is to contact your veterinarian to have them advise you on next steps.
Monitoring Diabetic Pets
Diabetic patients should be closely monitored. This will include monitoring of symptoms, body weight, appetite, thirst, and the amount of urine excreted. Your veterinarian will typically monitor glucose levels with blood tests when your pet has started treatment with insulin.
Periodic monitoring throughout the life of a diabetic pet is important to ensure insulin dosing is effectively correcting patient hyperglycemia (high blood sugar levels). Your vet will recommend appropriate follow-up exams to ensure the dose of prescribed insulin is working, and provide dosing adjustments if needed.
Call your vet if:
- Severe side effects are seen (see above) or if you see or suspect an overdose
- Call your vet or pharmacist if you have additional questions or concerns about the use of insulin
Proper Storage of Insulin for Dogs and Cats
Refer to your specific insulin packaging for recommendations on storage instructions.
All unopened bottles of insulin should be stored in the refrigerator at consistent temperatures from 36 F to 46 F until the expiration date.
Exposure to high temperatures over 86 F or freezing temperatures below 36 F can alter the insulin and lower its ability to work.
If you have left your insulin out of the refrigerator, contact your veterinarian, pharmacist, or the insulin manufacturer for specific product recommendations.
Insulin manufacturers generally recommend that the product be used within four to six weeks of first puncture. Contact your veterinarian for specific information and before starting your insulin.
Insulin FAQs
How long does it take for insulin to work in dogs?
For most diabetic pets, improvement of clinical symptoms occurs quickly after insulin therapy has begun. However, it can take several weeks for a pet to fully adjust to insulin therapy.
Every pet responds to insulin therapy differently and frequent monitoring of glucose levels is required for all diabetic pets.
How long does it take for insulin to work in cats?
For cats, as well as dogs, some improvement to clinical signs can be noted quickly after insulin therapy is initiated. It can, however, take several weeks and multiple adjustments to a cat’s insulin dose until a cat becomes stable with their insulin requirements.
Will insulin make my pet sleepy?
Insulin should not make your pet sleepy; it is a naturally occurring hormone that their body produces to help them process sugar into energy.
However, having a dose of insulin that is too high for their current blood sugar levels may cause hypoglycemia (low blood sugar) and lethargy (fatigue).
How long after eating should you give a pet insulin?
Ideally, insulin should be administered to your pet immediately after their meal, but be sure to follow the recommendation from your vet.
How much does dog and cat insulin cost?
Insulin costs can vary greatly but typically range from $30–$300 per month depending on the type of insulin and dosage of the pet. If you have financial concerns, be sure to discuss those with your vet when determining the best insulin for your pet.
