Heartworm Disease in Dogs: Symptoms, Causes, and Treatment
knape/iStock / Getty Images Plus via Getty Images
Heartworms in dogs are a serious and potentially life-threatening condition caused by a parasite spread through mosquito bites. Once inside the body, heartworms grow and live in the heart, lungs, and blood vessels, leading to lasting damage, including death, if left untreated.
While some dogs may not show symptoms early, the disease can quickly become severe.
The good news is that heartworms in dogs are highly preventable with year-round medication and routine veterinary care.
Understanding how dogs get heartworms, the signs to watch for, and how prevention works can help protect your dog’s health.
Key Takeaways
- Heartworm disease in dogs is a serious, potentially fatal parasite infection spread by mosquitoes.
- Symptoms may not appear early on, but can progress to coughing, fatigue, and breathing issues.
- Treatment involves multiple veterinary injections to kill heartworms, an oral medication, and strict exercise restriction.
- Year-round heartworm prevention is the safest and most effective way to protect dogs.
- Annual testing is essential—even for dogs on prevention—to detect infections early.
Summary
Heartworm disease in dogs is caused by the parasite Dirofilaria immitis. It causes heartworm disease not only in dogs, but also in cats, ferrets, and other mammals.
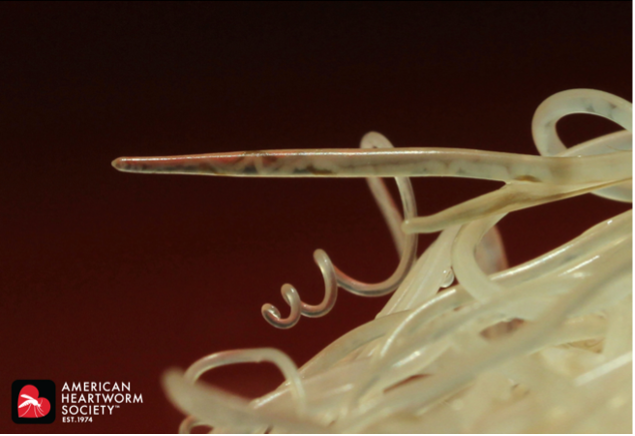
Heartworm is a large worm, reaching up to a foot or more in length. As it completes its life cycle—which takes about six to seven months—it ends up in an animal’s heart and pulmonary vessels, where it can live for several years.

As the heart becomes clogged with worms, there’s less blood it can push out to the rest of the body, and heart failure can result.
For PetMD's complete guide to heartworm disease in dogs, click here.
For the Spanish version, click here.
Symptoms
Severity of heartworm disease in dogs will be related to the symptoms present. Symptoms of heartworm in dogs are related to the organs affected—the heart and lungs.
Symptoms often include:
-
Exercise intolerance
-
Sudden death
Some dogs may show weight loss, difficulty breathing, and even excessive panting. If left untreated, dogs may go on to experience right-sided heart failure and ascites.
Causes
Heartworms are transmitted by mosquito bites. Dogs cannot get heartworm disease directly from one another.
As mosquitoes bite and take blood from an infected host (such as another dog, fox, wolf, or coyote), they ingest young immature heartworms (microfilariae). Inside the mosquito, these microfilariae mature into larvae.
When the same mosquito bites a dog, the larvae are spread into the dog’s blood, mature further, and travel to the heart, lungs, and blood vessels where they live.
Once they reach adulthood, female heartworms begin producing microfilariae, which begin to circulate through a dog’s bloodstream. This whole process takes about seven months to complete.
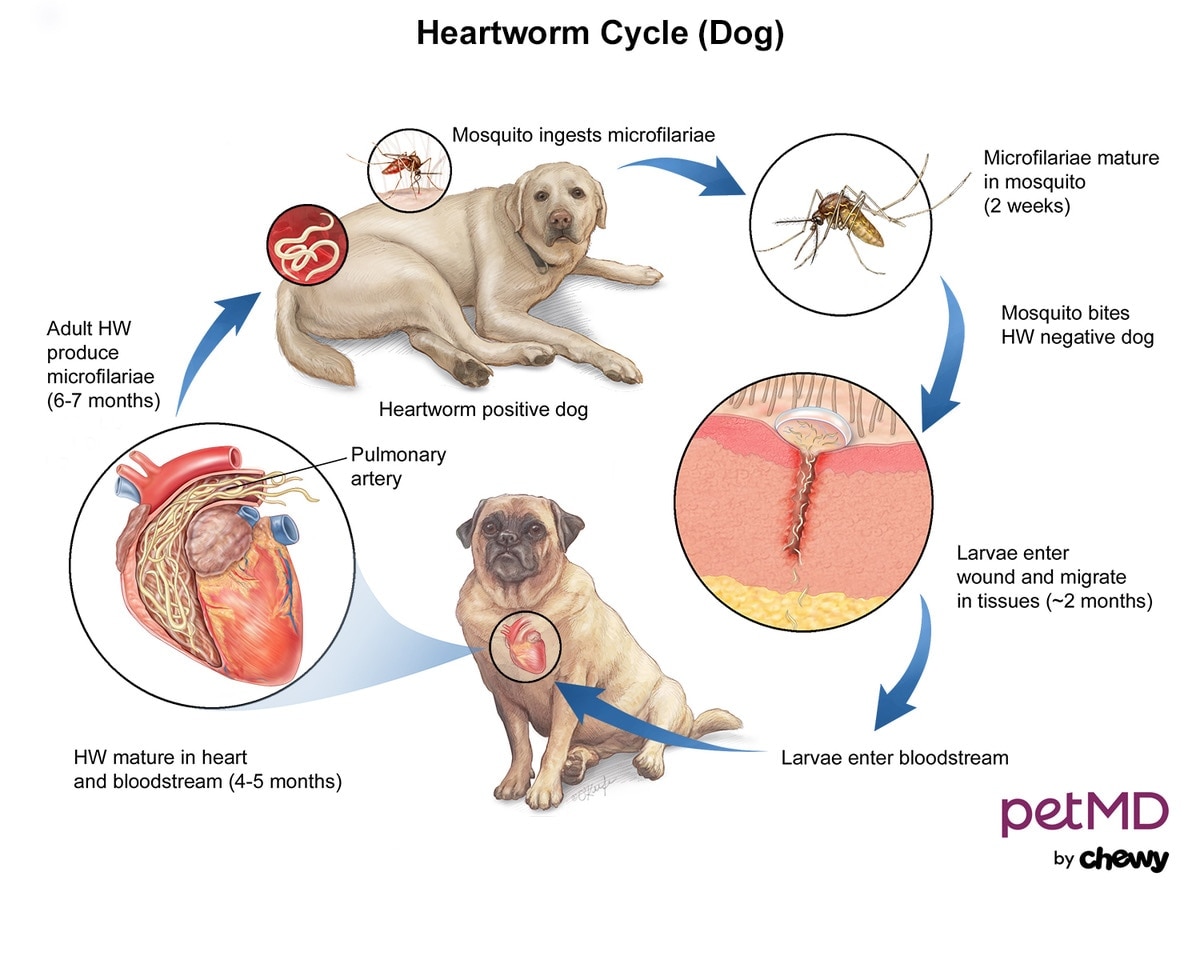
Click here to download this medical illustration.
Diagnosis
Dogs 7 months and older should be tested for heartworm disease at least annually.
If a dog misses a dose of prevention, then they should be tested more frequently. Testing is often done in the veterinary clinic and requires a small amount of blood.
The most widely used method for diagnosing heartworm disease in dogs is antigen-based testing. Antigens are proteins uniquely found on the surface of an organism that are used to detect the presence of that organism in the sample. In this case, the antigens being tested for are produced by the female adult heartworm, and if the test shows positive, then the dog is infected.
Other tests that can be performed include a blood smear or a modified Knott’s test (often a test that is sent to a special lab for diagnosis), which are done to check for the presence of circulating microfilariae.
Once a diagnosis is made, your veterinarian may recommend more testing, which is used to find out the severity of the infection as well as the amount of risk involved for treatment.
Other testing for the severity of heartworm in dogs may include:
-
Chest radiographs to identify heart enlargement, inflammation, and signs of heart failure
-
EKG to check the heart rhythm
-
Blood pressure
-
Cardiac enzyme evaluation (NT-proBNP) to identify the severity of heart failure
-
Echocardiogram to check how the heart pumps and identify any obstructions (such as heartworms)
-
Additional blood work to assess blood cells and other organ functions
-
Urine testing (urinalysis) to check for protein in the urine as a result of the immune system’s response to heartworm infection
Class I dogs are those with the lowest amount of risk for treatment, and Class IV dogs are those often diagnosed with caval syndrome and are at highest risk.
Caval syndrome occurs when the worm burden is so great that the worms are blocking blood from exiting the heart and the dog collapses. These dogs are dying and require surgical removal of the worms (often done by a specialist) to survive.
Treatment
Once your dog is diagnosed, your veterinarian will most likely explain to you next steps, including treatment options, more diagnostics, and time frame for follow-up visits.
Certain medications may be prescribed, such as:
-
Steroids: To decrease inflammation created by the worm itself
-
Antibiotics: Doxycycline is used to kill Wolbachia, an organism that lives within the heartworm. Without this organism, the heartworm becomes easier to kill, and secondary inflammation is minimized.
-
Specific heartworm preventive: To prevent younger worms from developing into adults and to rid the bloodstream of any circulating microfilariae
-
Melarsomine injections: Typically given by your vet at 30 days, 60 days, and 61 days to kill adult heartworms. It’s usually administered in the lower back deep into the muscle. As it is painful, pain medications will most likely be sent home at those visits as well.
In addition, you should limit your dog’s activities as exercise can increase the potential for the heartworms to dislodge and cause clots elsewhere in the body. If your dog has circulating microfilariae in their bloodstream, mosquitoes can spread infection to other dogs, so reducing outdoor exposure during treatment is recommended.
Nine months after treatment is completed, your vet will test your dog for heartworms to ensure that the treatment has been successful. It’s important that during this time and routinely thereafter, your dog is on heartworm prevention to prevent reinfection.
Prevention
Heartworm disease in dogs is prevented with year-round heartworm prevention medication and annual heartworm testing. Taking steps to avoid mosquito exposure can also help.
Heartworm Prevention for Dogs
Keep your dog on a vet-recommended heartworm prevention year-round and stay consistent with dosing—missing even one dose can increase your dog’s risk. There are multiple types and forms of heartworm prevention on the market, including:
-
Oral medications: Monthly chewable tablets
-
Topical treatments: Monthly liquid applied to the skin
-
Injectable prevention: Long-acting shot given by a veterinarian (typically every 6–12 months)
There are even products that are combined with flea and tick control to give your dog a more comprehensive preventive profile. Credelio Quattro, for example, is a monthly prescription flea and tick medication that also prevents heartworm disease, as well as treats and controls roundworms, hookworms, and tapeworms.
If your dog is already on a flea and tick preventive, your vet may prescribe Heartgard Plus, a monthly chewable that prevents heartworm disease, and treats and controls roundworms and hookworms.
Annual Heartworm Testing
Schedule annual heartworm testing, even if your dog is on prevention. Dogs on prevention still need yearly testing because:
-
Heartworm preventives do not kill adult heartworms
-
Missed or delayed doses can allow infection to develop
-
Early detection helps prevent serious complications
If your dog tests positive for heartworm disease, talk to your vet about the specific type of preventive needed while treating it—there are only a few that should be given to minimize secondary complications.
Reduce Mosquito Exposure
It only takes one infected mosquito to cause heartworm disease. Limiting your dog’s exposure to mosquitoes can help reduce risk, but in some places, limiting exposure is nearly impossible.
Avoid standing water and limit outdoor time at dawn and dusk when mosquitos are most active. In addition, spray your yard with a pet-safe mosquito repellant such as Wondercide. Check with your veterinarian before using additional repellents.
Recovery and Management
Treatment for heartworm disease is not risk-free.
Dogs that undergo heartworm treatment can suffer from:
-
Emboli (clots)
-
Sudden death
-
Possible formation of an abscess (pocket of pus) at the site of melarsomine injection
-
Emotional distress from months of exercise restriction
Dogs can also suffer from long-term health risks from the damage caused by the worms to their heart and lungs.
Scarring and inflammation (swelling) generated by the worms makes it difficult for blood to be pumped through the heart and lungs, and right-sided heart failure can develop, even with successful treatment.
The degree of severity will affect the prognosis, and the sooner the disease is caught and treated, the greater likelihood there is for a good outcome.
Unfortunately, dogs that suffer from heartworm disease don’t get immunity and are at risk for becoming infected again in the future—that’s why year-round prevention is critical for your dog’s health.
Prevention is key to stop heartworm disease from starting in the first place. Your veterinarian can help you determine which heartworm preventive medication is best for your pup based on their age and health.
Always speak with your veterinarian before starting a new medication for your dog. They will help you determine the best medication based on your dog's health.
Heartworm Disease in Dogs FAQs
How common is heartworm in dogs?
Heartworm disease in dogs occurs in all 50 states but is most common in warm, humid regions with high mosquito populations, such as the southeastern United States. Cases continue to rise nationwide, which is why veterinarians recommend year-round heartworm prevention for all dogs.
How do I check if my dog has heartworms?
To check for heartworm disease in dogs, a veterinarian performs a blood test that detects adult heartworms. Some clinics run the test in-house, while others send samples to a lab. In certain cases, a microscope exam may identify microfilariae (baby heartworms) in the blood.
Can a dog survive heartworm disease?
Yes, many dogs can survive heartworm disease with prompt veterinary treatment, but outcomes depend on how advanced the infection is. Early-stage cases have a good prognosis, while severe cases can be life-threatening. Treatment is intensive and carries risks, which is why prevention and early detection are critical.
